Introduction
Running is a popular sport, and more and more people are taking up running. The Rotterdam Marathon is considered by many to be the most beautiful running event in the Netherlands.
Although the race takes place in April, when temperatures often seem mild, the organization increasingly sees runners getting into trouble due to heat.
In this article, we explore why this happens and how to prevent it.
Background
Body temperature is tightly regulated around 37 °C. When it rises above 40 °C, risks increase. At temperatures above 42 °C, irreversible damage occurs.
The body constantly works to maintain a balance between heat production and heat loss. Heat is produced in the muscles and organs such as the liver and brain. The environment also plays a role: sometimes it adds heat, and sometimes it helps remove it.
The body loses heat in several ways. Heat escapes through radiation from the skin, through contact with cooler surfaces (conduction), through moving air (convection), and most importantly through sweating (evaporation). Sweat evaporates and carries heat away, allowing the body to cool itself.
However, the body is not very efficient in its use of energy. Approximately 80% of the energy used during exercise is converted into heat, and only 20% contributes to forward movement.
The increase in heat production during exercise is significant. At rest, the body produces about 100 watts of heat — similar to a light bulb. During intense exercise, this can rise to 1000 watts, comparable to a space heater.
Without adequate cooling mechanisms, body temperature can rise by 1 °C every five minutes. That means it may exceed 40 °C within fifteen minutes and surpass 42 °C within half an hour.
It is therefore not surprising that body temperature rises during exercise. A study during the Seven Hills Run showed that more than half of finishers had a body temperature of 39 °C. Participants swallowed a pill that measured core temperature. While this is not inherently dangerous, maintaining a stable temperature improves performance.
Environmental Temperature
The temperature reported in weather forecasts reflects only the thermometer reading taken in the shade. What runners actually experience is the “feels-like” temperature.
This “feels-like” temperature depends on several factors: air temperature, solar radiation, humidity, and wind speed.
To illustrate, a sauna at 100 °C with 20% humidity can feel as stressful as a steam room at 40 °C with nearly 100% humidity.
The scientific term for this combined heat stress is the Wet Bulb Globe Temperature (WBGT). In simple terms, it tells you how stressful the heat really is for the body. The higher the WBGT, the greater the risk.
Heat Illnesses
The combination of exercise and rising environmental temperatures increases the risk of heat-related illnesses. These range from mild to life-threatening. In this article, we focus on the two most serious forms: heat exhaustion and exertional heat stroke.
Heat Exhaustion
Heat exhaustion is a condition in which the athlete can no longer continue exercising.
Body temperature is usually above 38 °C. Symptoms may include general weakness, impaired coordination, nausea or vomiting, heavy sweating, increased heart rate, rapid breathing, and low blood pressure.
Blood tests may show dehydration and electrolyte disturbances. Consciousness remains (almost) normal.
Exertional Heat Stroke
The most dangerous heat illness is exertional heat stroke (heat stroke). It is defined as a core body temperature above 40 °C combined with altered mental status. This is a life-threatening condition.
Physical signs may include an increased heart rate, rapid breathing, and low blood pressure. Nausea and vomiting can occur, and coordination may be impaired.
The most critical feature is reduced or lowered consciousness. This may begin subtly with confusion or difficulty answering simple questions. In more severe cases, it can progress to irrational behavior, emotional instability, fainting, decreased responsiveness, or seizures.
From the outside, overheating is not always obvious. Some athletes feel hot and sweat heavily. Others may feel dry and cool to the touch because of severe fluid loss, even though their core temperature remains above 40 °C.
And it is not rare. Heat stroke remains one of the more common causes of death among young athletes. According to the CDC, hundreds of heat-related deaths are reported annually in the United States. The risk strongly correlates with WBGT.
How Does Exertional Heat Stroke Develop?
Exertional heat stroke occurs when the body produces more heat than it can dissipate.
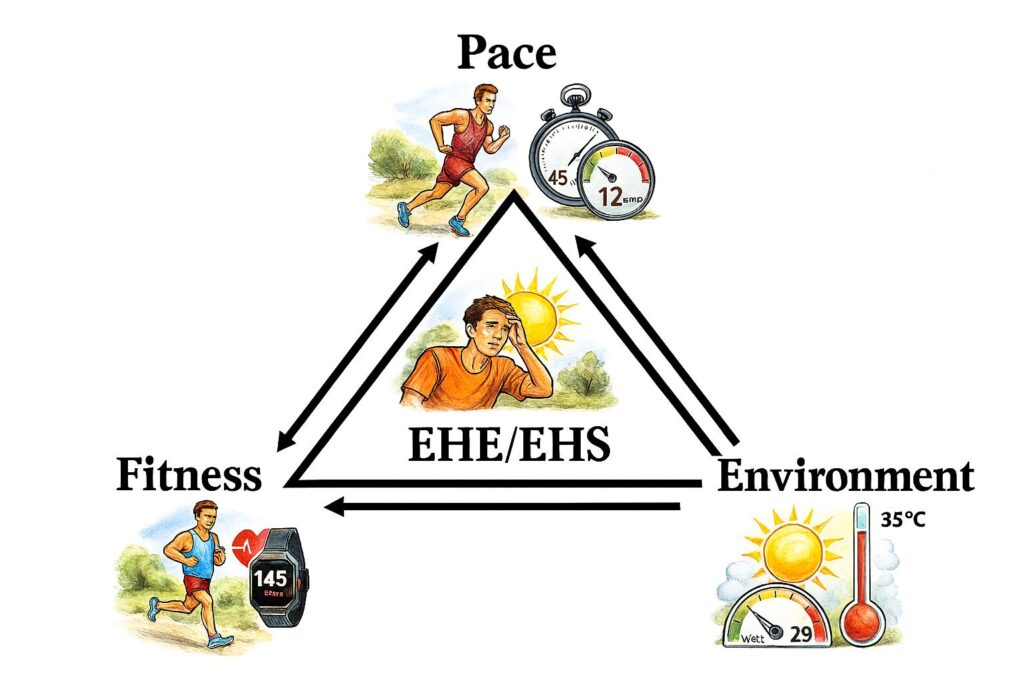
Three things matter: fitness, environmental heat stress, and pace. When these three factors are out of balance, risk increases.
Fitness
Even well-trained runners can have an “off” day. Poor sleep, illness, stomach problems, hydration status, and certain medications all influence performance and heat tolerance.
Environmental Heat Stress
If runners are not accustomed to the current heat conditions, risk increases. When temperatures in the two weeks prior to the race were lower than on race day, the body is not fully adapted.
This process of adaptation is called acclimatization. Full heat acclimatization typically takes about two weeks.
Pace
The chosen speed must be realistic. If the pace is too ambitious, or if conditions or fitness change, risk increases.
The body gives warning signals. Ignoring them increases danger. This is more common in younger runners (under 35), less experienced athletes, and those chasing an unrealistic time goal.
Tips to Prevent Heat Stroke
To reduce risk, the athlete should train adequately, set realistic goals, stay properly hydrated, wear appropriate layered clothing, and adapt the race plan to the conditions.
Being acclimatized to heat is an advantage. Training in warm conditions improves tolerance and does not disadvantage runners in cooler weather.
Environmental conditions cannot always be replicated in advance. Specific heat training may include wearing extra layers during sessions or applying controlled heat exposure afterward, such as taking a warm shower or bath.
Most importantly, be willing to adjust. Conditions change. The body changes. The race plan should change too.
Finishing safely is more important than chasing an unrealistic time.
Treatment of Exertional Heat Stroke
Prevention is better than cure. Awareness of risk and early recognition are essential.
Any athlete with reduced or lowered consciousness after intense exercise should be considered as potentially having heat stroke. Seek immediate medical assistance.
At organized events, alert medical staff. Otherwise, call emergency services. Medical professionals will confirm the diagnosis by measuring core temperature.
If heat stroke is suspected, cooling must begin immediately. Move the athlete to shade. Remove excess clothing. Start cooling at once.
Cooling someone who ultimately does not have heat stroke is less harmful than failing to cool someone who does.
At medical stations, ice-water immersion or ice-soaked towels are used. If unavailable, any cooling is better than none. Wet the skin with water, use a hose, or fan the athlete.
Continue cooling until medical help arrives. The athlete should then be transported to a medical facility for further care.
Conclusion
Running has many benefits for both mental and physical health. However, rising global temperatures mean heat-related risks are increasing.
In exertional heat stroke, core temperature rises above 40 °C and mental status changes. This is a medical emergency requiring rapid recognition and action.
Recognize the warning signs. Act quickly. Adjust the pace. Finish safely.